Illustration by Marta Pucci
Progesterone 101
Getting to know our hormones.

Top things to know about progesterone:
Progesterone levels fluctuate throughout the menstrual cycle
Levels are highest after ovulation
Progesterone is necessary for conception and helps maintain a pregnancy
What is progesterone?
Progesterone is a key hormone belonging to a group called progestogens (1). Hormones are small molecules produced by glands in your body (2). They travel through the bloodstream until they reach an organ with receptors designed for them. They bind to that receptor, enabling communication between cells in the body (2).
Progesterone is a sex hormone (just like estrogen or testosterone), so it affects sexual development during puberty and is also involved in becoming pregnant (3).
Progesterone targets and impacts various parts of the body, including the uterus, vagina, cervix, breasts, and testes, as well as the brain, blood vessels, and bones (2,4).
Understanding the importance of progesterone and how it affects your body at different stages of life can help you better manage menstrual symptoms, recognize when something isn’t right, support a healthy pregnancy, and make informed choices about birth control. This understanding can also help you advocate for yourself with your healthcare provider.
How is progesterone produced?
Your body uses cholesterol (a fat molecule) to make progesterone (2). Progesterone is mainly produced in the ovaries by the corpus luteum (5), which is the structure that develops after ovulation when the follicle collapses around the egg. The adrenal glands (located on top of the kidneys) also produce some progesterone (2).
During pregnancy, the main sources of progesterone are initially the corpus luteum and—after 10 weeks— the placenta (6,7).
What does progesterone do to the body?
Progesterone plays several important roles in the body. It:
Stops the build-up of the endometrium (uterine lining) caused by estrogen
Reduces cervical mucus production
Inhibits ovulation when at high levels
Prepares the endometrium for the possible implantation of a fertilized egg
Supports and helps maintain early pregnancy
Develops the mammary glands (breast tissue) during pregnancy in preparation for lactation
Relaxes the uterus to prevent contractions during pregnancy
Decreases activity in the intestines, possibly causing constipation (2,4,6,8,9)
How do progesterone levels change during the menstrual cycle?
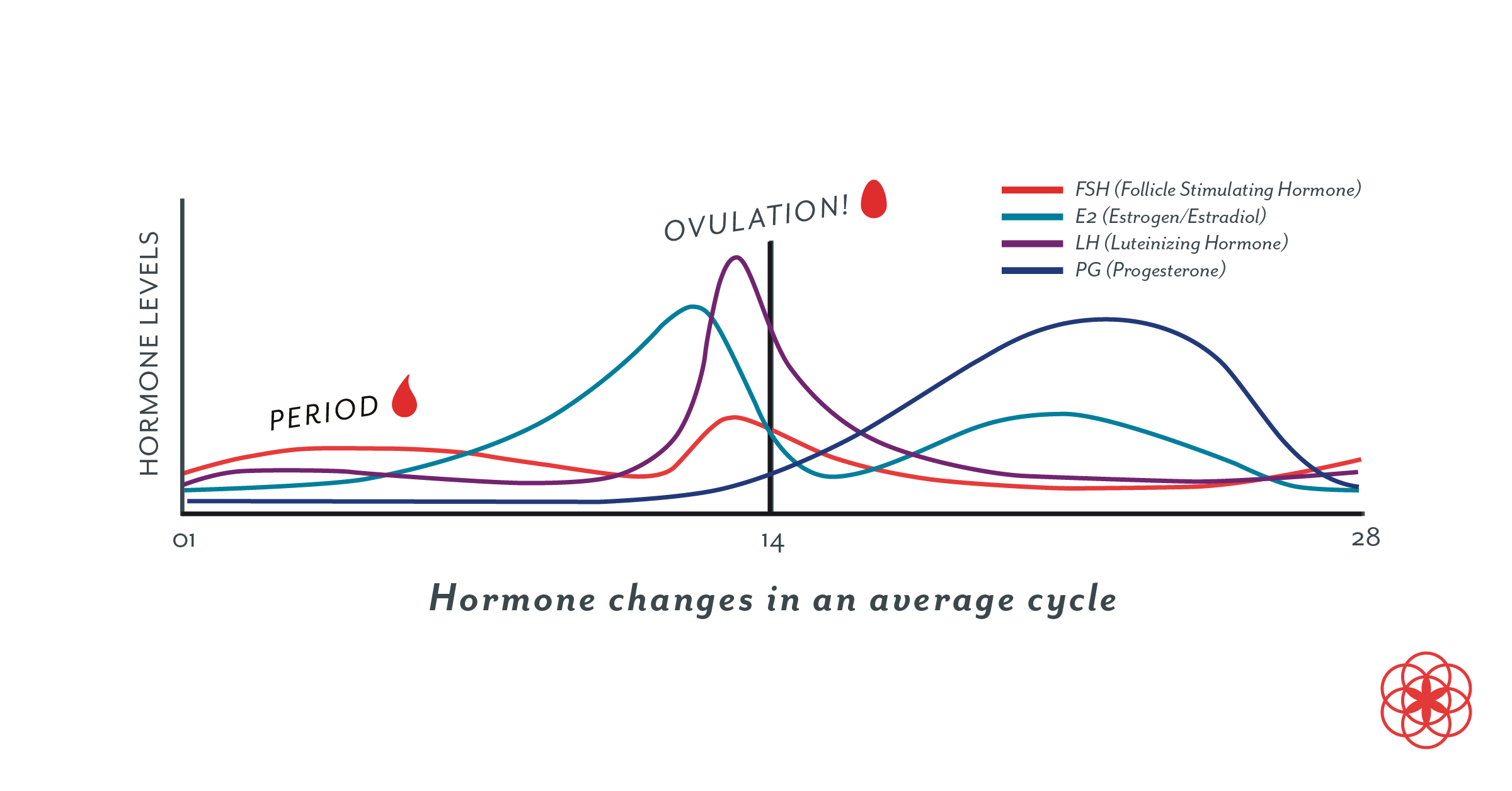
Progesterone levels are not fixed. They vary throughout the menstrual cycle and can change depending on the specific phase of the cycle you’re in (10).
Before ovulation = lower progesterone
Progesterone levels are low at the beginning of the menstrual cycle (during your period) and remain low throughout the follicular phase, which is the time before ovulation occurs (6,11).
After ovulation = higher progesterone
Progesterone levels are highest in the middle of the luteal phase. This is after ovulation and before menstrual bleeding begins. Progesterone is produced by the corpus luteum (the structure that forms in the ovary after ovulation) (12,13). If pregnancy does not occur, the corpus luteum begins to break down 9–10 days after ovulation, causing progesterone levels to fall and menstrual bleeding to begin (2,6).
How do I know if my progesterone levels are normal?
You may notice some signs and symptoms if your progesterone levels aren’t within the typical range, whether this is too high or too low.
Low progesterone
Progesterone may be low if ovulation is not occurring regularly (or at all), or if your body cannot produce enough progesterone.
Some signs and symptoms of low progesterone include:
Long or heavy periods
Spotting before your period
Short menstrual cycles due to a short luteal phase (6,14)
Some conditions, such as elevated prolactin (a hormone that induces milk production), hypothyroidism, or polycystic ovary syndrome (PCOS), can cause infrequent or absent ovulation, which would lead to low progesterone levels (15). In these cases, the cause of the low progesterone should be diagnosed and treated, so it’s a good idea to see your healthcare provider.
Luteal phase defect
Luteal phase defect is a condition where the body does not produce enough natural progesterone so that the endometrium (lining of the uterus) can support the implantation and growth of an early pregnancy (16). This is also called luteal phase insufficiency. Diagnosing a luteal phase defect can be difficult, as there's no single agreed-upon test for it.
When there is no known cause for low progesterone, there are no clear guidelines on how and when to treat it. In general, there is little information available about people who have low progesterone and are not trying to become pregnant (17).
Is there a link between low progesterone and miscarriage?
Since progesterone is important for early pregnancy, it might seem that low levels could contribute to infertility or lead to miscarriage (18). However, it’s debated whether a luteal phase defect is a cause of infertility or not, along with how best to diagnose and treat it (16).
Research has shown a link between low progesterone levels and early miscarriage, and low progesterone levels may help identify pregnancies at risk of miscarriage (19,20). In one study of 929 pregnant individuals, progesterone levels steadily increased between weeks 5 and 13 in healthy pregnancies. In contrast, pregnancies that ended in miscarriage showed only a slight, non-significant rise in progesterone during that time. These findings suggest that progesterone plays an important role in early pregnancy and that low levels may signal a higher risk of pregnancy loss.
One study showed that people who experienced bleeding during early pregnancy had lower progesterone levels and were more likely to have a miscarriage than people who didn't experience bleeding in the first trimester (21).
However, there is currently no evidence that taking supplements of progesterone lowers the risk of miscarriage. Therefore, progesterone supplementation is not routinely used to prevent early pregnancy loss. A healthcare provider may recommend the use of progesterone depending on the individual circumstances (22,23).
Low progesterone in early pregnancy may be a symptom of a pregnancy that isn’t viable, versus the cause of miscarriage. Research also found that chromosomal abnormalities in the fetus may be linked to changes in progesterone levels. It has been shown that progesterone levels may be lower in pregnancies affected by trisomy 13 and trisomy 18 (21).
High progesterone
Elevated levels of progesterone are uncommon, but in rare cases, it can be a sign of certain conditions, such as:
Congenital adrenal hyperplasia (CAH)
A type of abnormal pregnancy called a hydatidiform mole
Some ovarian cysts
Certain ovarian tumors (24)
If you think your progesterone levels may be too high, it’s best to talk to your healthcare provider. A simple blood test can show whether your progesterone levels are within the typical range.
What are typical levels of progesterone during different life stages?
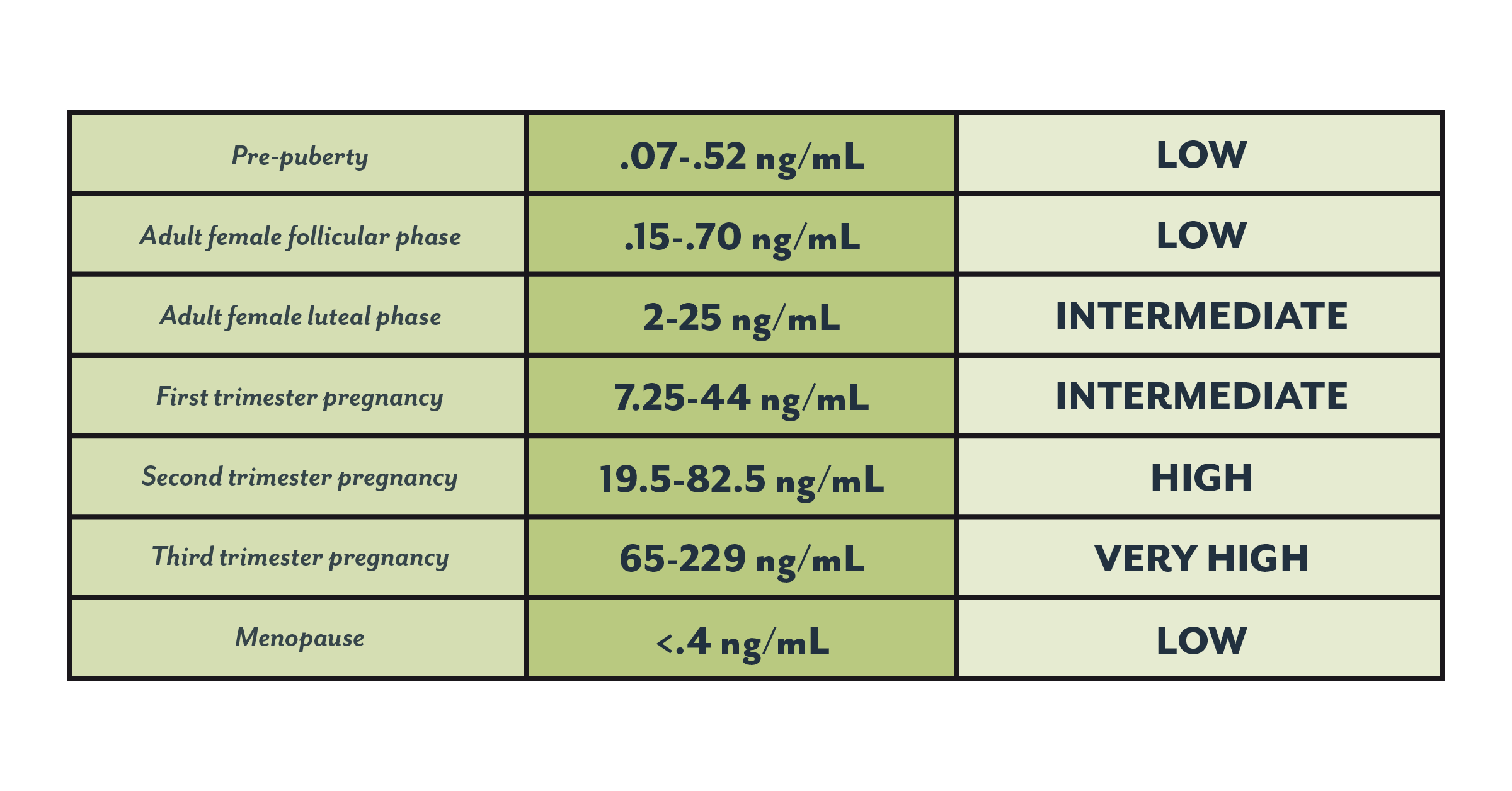
Progesterone levels can vary from person to person, but also from cycle to cycle (17). Differences in laboratory procedures, population served by the laboratory, and testing technique can also impact results, so results should always be interpreted using the laboratory’s reference values (11).
Here’s a progesterone levels chart to give you an idea of how levels compare across different life stages (24). You might want to bring this with you to any appointments to compare with your healthcare provider.
How does hormonal birth control affect the progesterone in my body?
Your progesterone levels while taking hormonal birth control will depend on whether your method blocks ovulation. If you’re not ovulating, then your progesterone levels will be low and flat (no peak).
Regardless of what type you’re on, most hormonal birth control contains progestin, which plays a key role in what’s happening.
What is progestin?
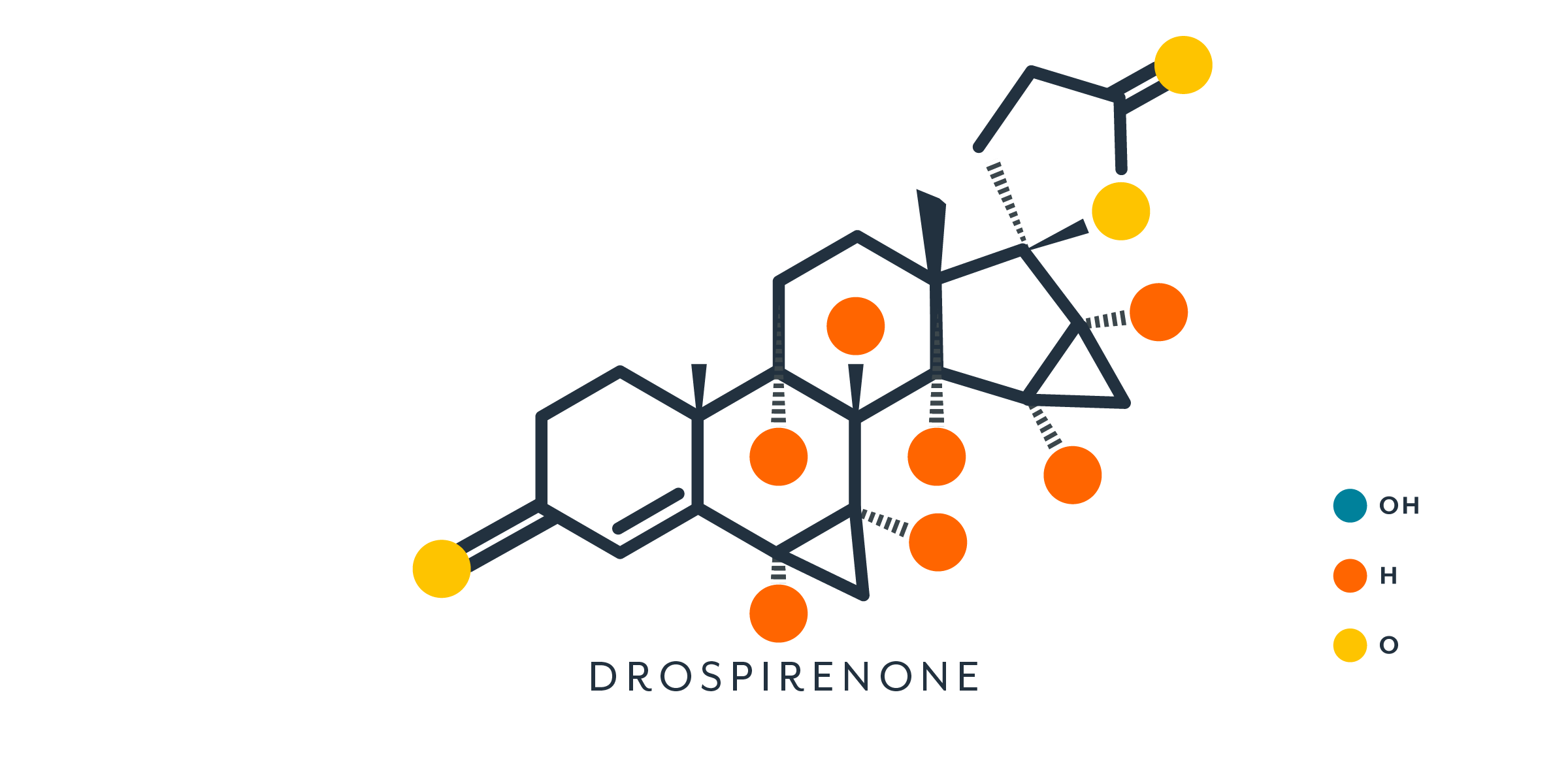
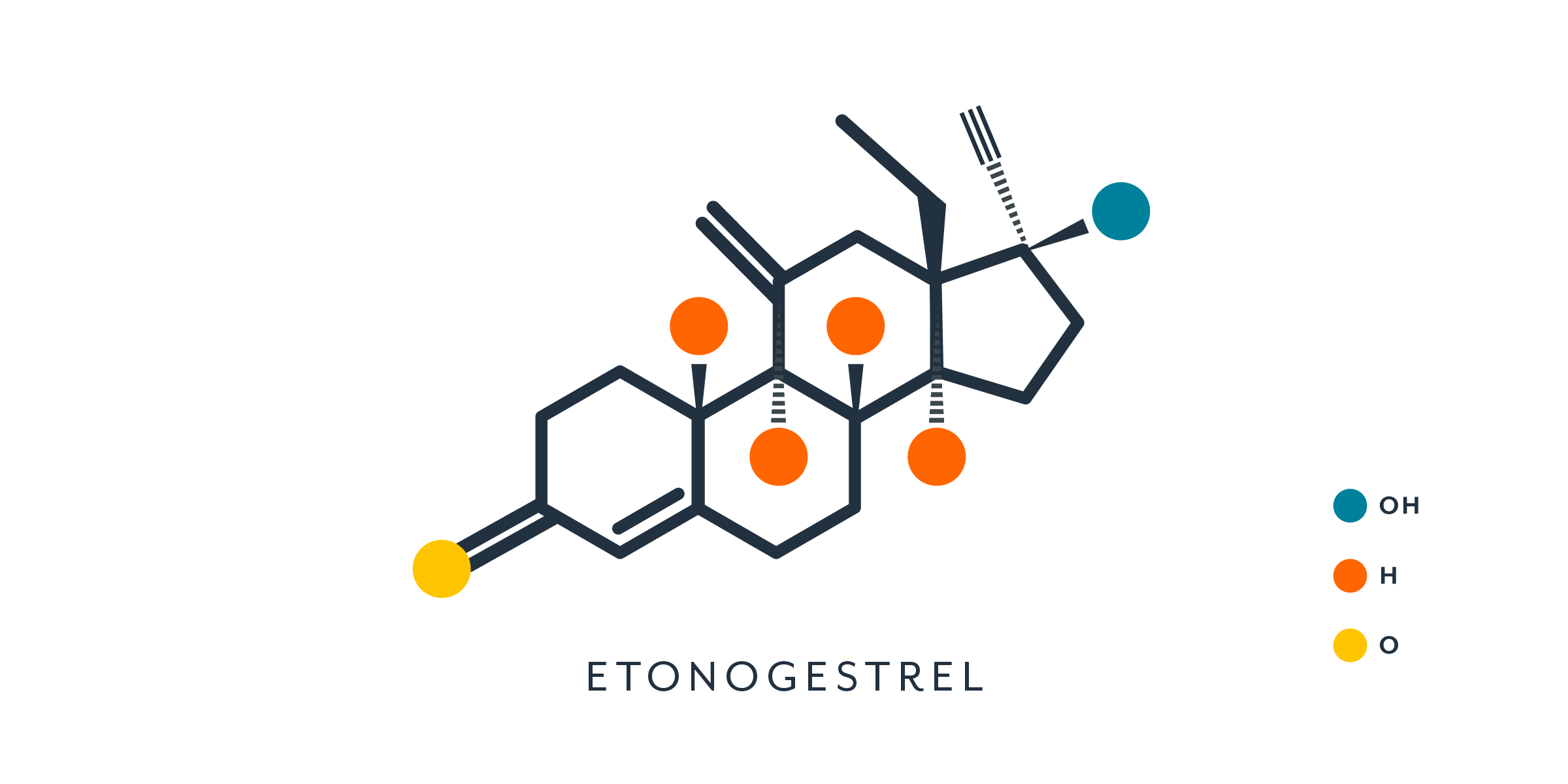
Progestins are synthetic hormones made from progesterone or testosterone that have progesterone-like effects (25). Progestins are used in all hormonal contraceptives (either alone or in combination with an estrogen) and some menopausal hormone therapies.
Due to slight differences in their chemical structure, progestins do not fit perfectly onto progesterone receptors and may also bind to other receptors, leading to potential side effects (4). Some people may experience hirsutism (excess hair) or acne, especially if the birth control contains little or no estrogen (14). Not everyone's response will be the same, but for some people, the formulation and type of progestin can make a difference.
Sometimes the dose of progestin isn't high enough. This can cause bleeding or spotting while still taking active (hormonal) birth control pills, or cause heavier periods (14). A change in dose or type of birth control may improve these side effects. However, it may not always be the progestin that’s causing the problem. With combined hormonal contraceptives, the dose of estrogen may also play a role in some side effects.
If you have an unwanted side effect that you think may be related to your birth control, talk to your healthcare provider. Using Clue to track your cycle can help you see if there's a pattern to what you're experiencing.

Combined hormonal contraception
Combined hormonal contraceptives include both a form of estrogen and a progestin, and they primarily prevent pregnancy by stopping ovulation. They also work by thickening cervical mucus (26).
The pill
Progesterone is suppressed in people who take combined oral contraceptives (COCs) like the pill (various doses, progestin types, and regimens), indicating that ovulation does not typically occur with this method (27,28).
The patch
A study found that progesterone levels for people using the birth control patch were lower than they were before starting the patch (29). The patch prevented ovulation in almost all cycles when used correctly.
The ring
In a study of 21 contraceptive ring users, progesterone levels were consistently low (on average <0.63 ng/mL) because no ovulation occurred over 2 months of use (28).
Progestin-only contraception
Ovulation may still occur on some progestin-only birth control methods. This means that progesterone levels will still rise and fall in the same way they do for people not on hormonal birth control. Ovulation rates among this group vary because, although all the birth control methods contain a progestin, there are different types and dosages, and they enter the body through different routes (4). This affects the amount of progestin that makes it into the bloodstream and up to the brain to stop ovulation.
Just because ovulation may still occur on this type of birth control, this doesn't mean that the birth control isn’t working. Progestin-only methods also work in other ways, such as thickening cervical mucus and blocking sperm from reaching the egg (26).
The implant
The majority of implant users do not ovulate (26). The implant thins the uterine lining and thickens the cervical mucus. A study followed 7364 implant users for 36 months during use and for 6 months after removal. Only three pregnancies occurred while the implant was in place, and a further three happened within a week of its removal. This shows that the implant is highly effective at preventing pregnancy. The likelihood of becoming pregnant while using the implant is very low, approximately 4 in every 10,000 users per year (30).
Ovulation is common among people using hormonal IUDs. In a small study of 10 people using the 52 mg levonorgestrel IUD, ovulation occurred in almost half the cycles, but this number increased over time (31).
In a study of 14 people using the 52 mg levonorgestrel IUD for 6 years, ovulation occurred in 79% of the cycles even though nine of the study participants did not have regular periods (32). In those who ovulated, progesterone levels followed typical progesterone patterns, peaking on cycle days 20–25 at typical levels (24,31,33).
For people using the lower-dose hormonal IUDs (19.5 mg and 13.5 mg types), ovulation occurs in almost all cycles (26).
IUDs are highly effective even when ovulation occurs, as they prevent sperm from fertilizing the egg (26).
The shot
The contraceptive injection or shot—a medication known as the depot medroxyprogesterone acetate (DMPA) injection—inhibits ovulation and therefore suppresses ovarian progesterone production (26).
The average progesterone level for someone using the contraceptive injection is 0.40 ng/mL, (34). This level is similar to someone who is not on any form of hormonal birth control and is in the follicular (pre-ovulatory) phase of their cycle (24).
Progestin-only pill (“mini-pill”)
The progestin-only pill inhibits ovulation, although it does not do so consistently. Approximately 4 out of 10 people using a progestin-only pill still ovulate. Additionally, this pill thickens the cervical mucus, making it harder for sperm to enter the uterus and fertilize a potentially released egg (7).
Another result of progestin-only pills is the thinning of the uterine lining (7). In a study of 43 people taking the mini-pill containing the progestin norethindrone, 60% had low progesterone levels without the typical peak, demonstrating either no ovulation or low progesterone production from the corpus luteum (35). The remaining 40% of people likely ovulated since they had a progesterone peak, just like people not on hormonal birth control (35). The likelihood of ovulation in this group remained the same at both 2 months and 6 months of use (36).
What else should I know about progesterone?
Progesterone and the abortion pill
The "abortion pill" (mifepristone) is a medication that blocks progesterone by binding to its receptor without activating it. This prevents progesterone from playing its normal role in early pregnancy, which is to help the embryo implant and keep the uterus from contracting (26,37).
Mifepristone is used along with another medication called misoprostol to induce elective abortions in the first trimester (37) but also to treat early miscarriages (38).
FAQs
On what days of the menstrual cycle is progesterone highest?
Every cycle is different, so the specific day that progesterone peaks can differ from person to person and cycle to cycle. Generally, the highest levels of progesterone occur around the middle of the luteal phase and peak 6–8 days after ovulation. Progesterone starts to drop in the days leading up to the period (39).
What is the ideal progesterone level needed to get pregnant?
For conception to occur, ovulation must take place. In a cycle where ovulation occurs, progesterone levels are usually above 7 ng/mL. In cycles that lead to pregnancy, progesterone levels are typically above 10 ng/mL. However, progesterone levels can fluctuate. A single measurement should be interpreted with caution (17,40).