Illustrations: Katrin Friedmann, Marta Pucci and Emma Günther
Ovulation: What is it, and how do I know when I'm ovulating?
Everything you've always wanted to know about ovulation

Top things to know about ovulation
Your eggs live in sacs in your ovaries, called follicles
Follicles need the right conditions to grow and release their egg: your environment, health, and behaviors all play a role
To know when you ovulate, you can track your cycle, cervical fluid, basal body temperature, and/or take ovulation tests
Ovulation is sometimes associated with ovulation bleeding or ovulation pain
What is ovulation?
Ovulation is the release of an egg from your ovary, into your fallopian tube. It typically happens about 13–15 days before the start of each period (1). Like your period, the timing of ovulation can vary cycle-to-cycle, and you may have the odd cycle where you don’t ovulate at all.
Understanding how ovulation works can be a powerful tool for your health
It’s common that people are introduced to the topic only after they have trouble becoming pregnant. But having a grasp on the process can give you insight into more than fertility. You’ll better understand any hormonally-influenced changes to your body around that time, and learn what factors might affect the timing of your ovulation (like stress), and why.
Research has found that in the global north, we ovulate roughly 400 times throughout our lifespan (2). This number is influenced by the use of contraceptives (many of which block ovulation), time spent pregnant and breastfeeding, and any behaviors or health conditions that affect the reproductive hormones (e.g. eating disorders, PCOS). Prehistorically, women would have ovulated less than half as often (3).
If conditions aren’t right, ovulation won’t happen
The development and release of an egg each cycle occurs in response to the intricate ups and downs of your reproductive hormones. Ovulation (and the menstrual cycle as a whole) is impacted by energetic, nutritional, emotional, and socioeconomic factors.
Short-term factors like jet lag, seasonal changes, stress, and smoking can have an effect, as well as longer-term factors like PCOS and thyroid disorders (4–8).
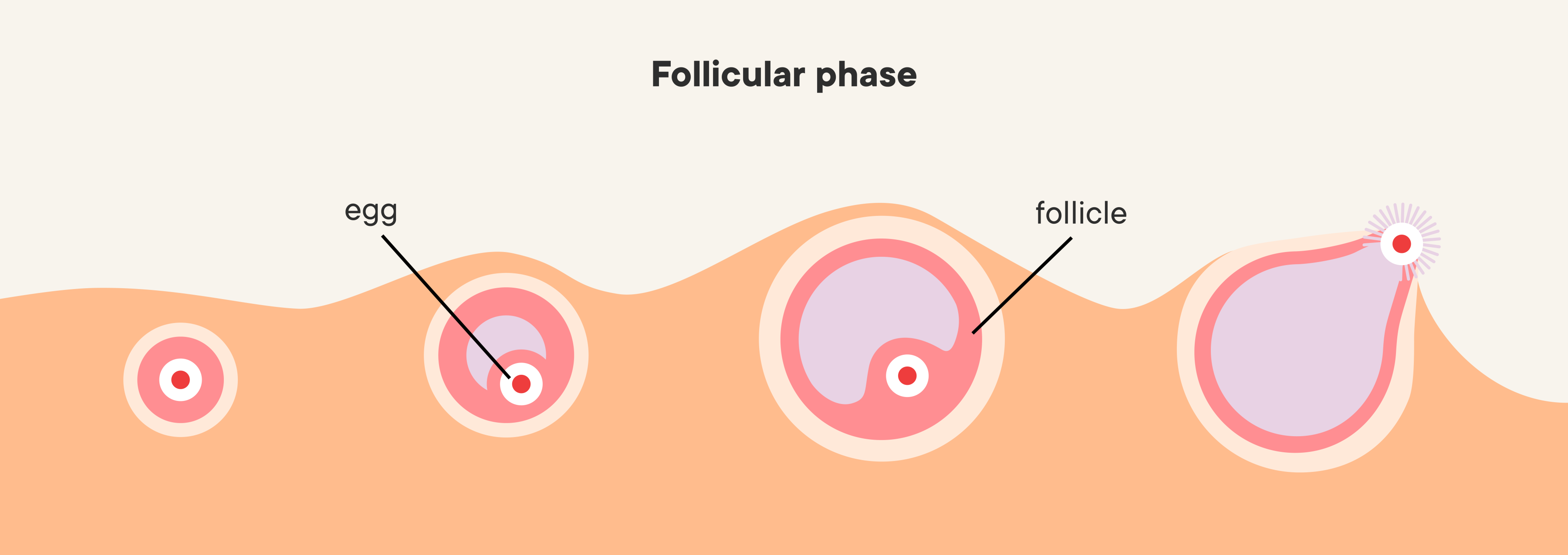
The basics of how ovulation works
Tiny eggs develop in sacs called follicles in your ovaries. Follicles develop for several months before they are ready to release their egg, (estimated at >175 days, or >~6 cycles) (9, 10). At any given time, there are follicles at several stages of development in your ovaries (10).
Early scientists once mistook the follicle for the egg itself
Follicles undergo incredible changes leading up to ovulation, developing many parts and layers, each with their own functions. Most follicles, though, will never reach ovulation, dying off at different phases of development or pre-development.
At the beginning of each menstrual cycle, a few (around 10) developing follicles are considered candidates for that cycle’s ovulation (11). By about midway through the follicular phase, one follicle becomes dominant.
Just like a superstar athlete being selected from the pack, all resources then go to preparing that single follicle, and the other potentials die off.
When the follicle is ready, it releases its egg. The egg travels out of the ovary and is taken up by the fallopian tube (the two aren’t actually attached—think of the end of the fallopian tube collecting the egg from the abdominal cavity). After its release, the egg has about 12–24 hours to be fertilized by sperm in the fallopian tube. If the egg isn’t fertilized within this short window, it begins to degrade. If it is fertilized, it travels to the uterus over the following 6-12 days, to possibly implant for pregnancy (12, 13).
All of these events are driven forward by the cyclical changes in your reproductive hormones. Hormones control the selection and development of your follicles, the release of each egg, and the preparation of your uterus for possible implantation.
This first part of the cycle is called the follicular phase (now you know where it gets its name).
How do your brain and hormones interact with ovulation?
The brain-ovarian connection that controls follicle development and ovulation is called the hypothalamic-pituitary-ovarian axis, or HPO Axis.
Before ovulation
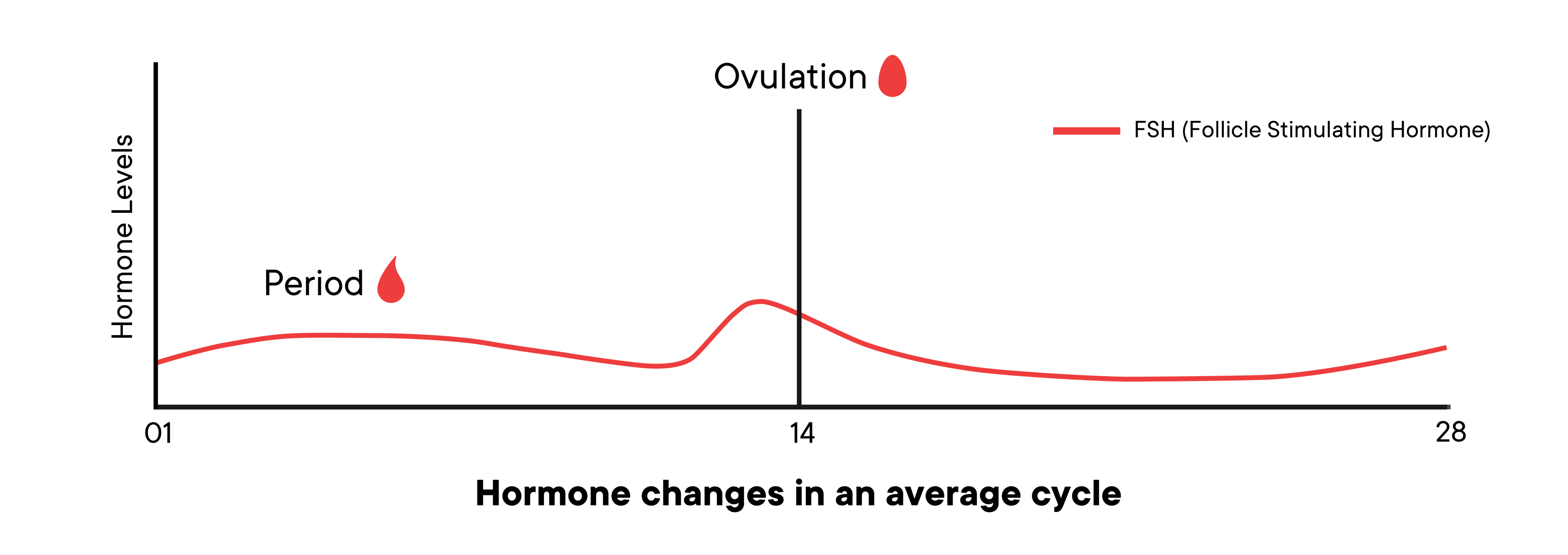
The brain produces continuous bursts of follicle-stimulating hormone, or FSH, throughout your cycle. FSH does exactly what it’s named for—it stimulates follicles to develop (2). As follicles grow, they produce estrogen.
As a dominant follicle is selected and grows (days 6–9 of the cycle), estrogen begins to spike (10).
A follicle becomes dominant at about 10mm in diameter, and typically grows to be about two centimeters in diameter (and up to about 3.3cm) (14–17). That’s about the size of a grape, or a hazelnut with its shell on.
Ready for release
When the amount of estrogen reaches its upper threshold, the egg is ready for release. The brain then produces a surge of luteinizing hormone (LH), triggering ovulation. The release of the egg from the follicle and ovary happens about 24 hours later (10–12 hours after LH peaks) (13, 17). The follicle uses enzymes to degrade its own wall and form an opening, allowing the release of the tiny egg from its center (18).
At the end of the fallopian tube, a finger-like structure swells with blood to grab and usher the egg in. Meanwhile, the egg has been undergoing its own changes to prepare for possible fertilization.
The pre-ovulatory follicle is the primary source of estrogen in the body. The dominant follicle is the source of more than 90% of the estrogen production in the pre-ovulatory period (19).
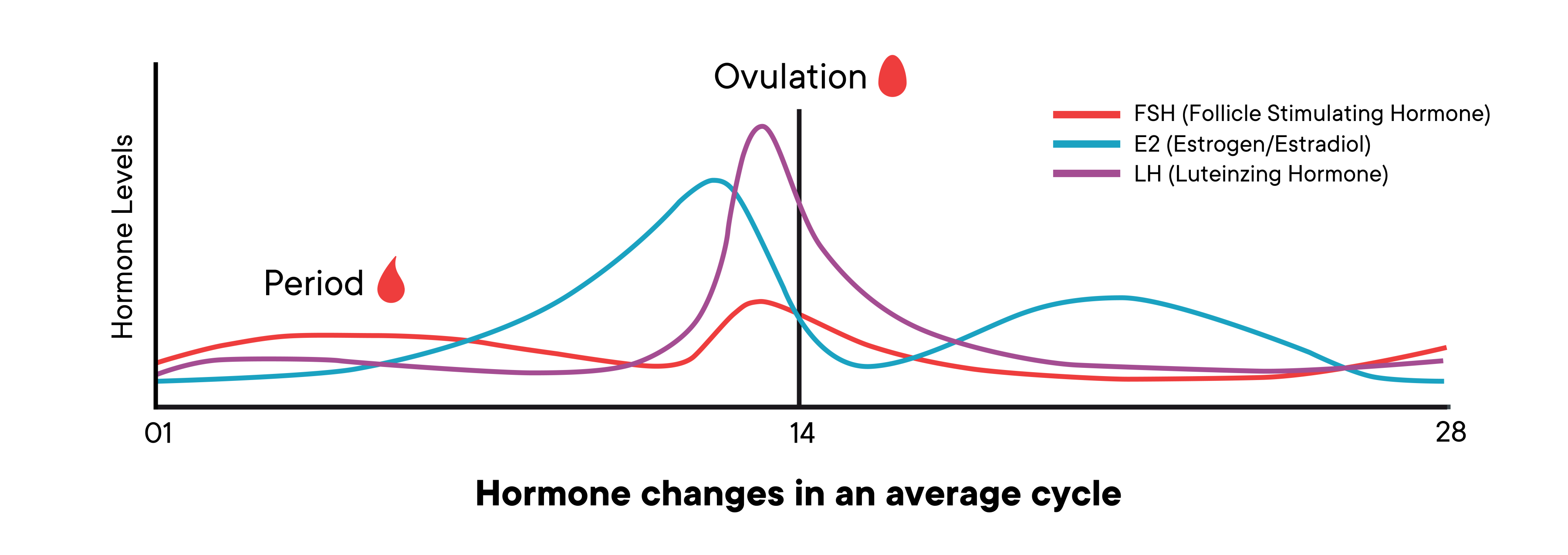
Take a look at the hormones graph. You’ll see estrogen, in blue, starts low and begins to spike midway through the follicular phase.
After ovulation
The egg may be on its way, but the follicle’s job is far from over. Luteinizing hormone transforms the large estrogen-making follicle into a progesterone-making machine (10).
This new progesterone producer (which also produces estrogen) is called the corpus luteum, or “yellow body” in Latin (because it’s yellowish in color). A new corpus luteum is made every cycle in which ovulation occurs. If ovulation doesn’t happen, you won’t get that surge in progesterone at all.
If the egg isn’t fertilized by sperm and then implanted in the uterine lining (after traveling down the fallopian tube, which takes several days), the corpus luteum begins to degrade, and hormone levels drop, triggering your period (20). If pregnancy does happen, the corpus luteum provides enough progesterone for your pregnancy to develop, until the placenta can take over (21).
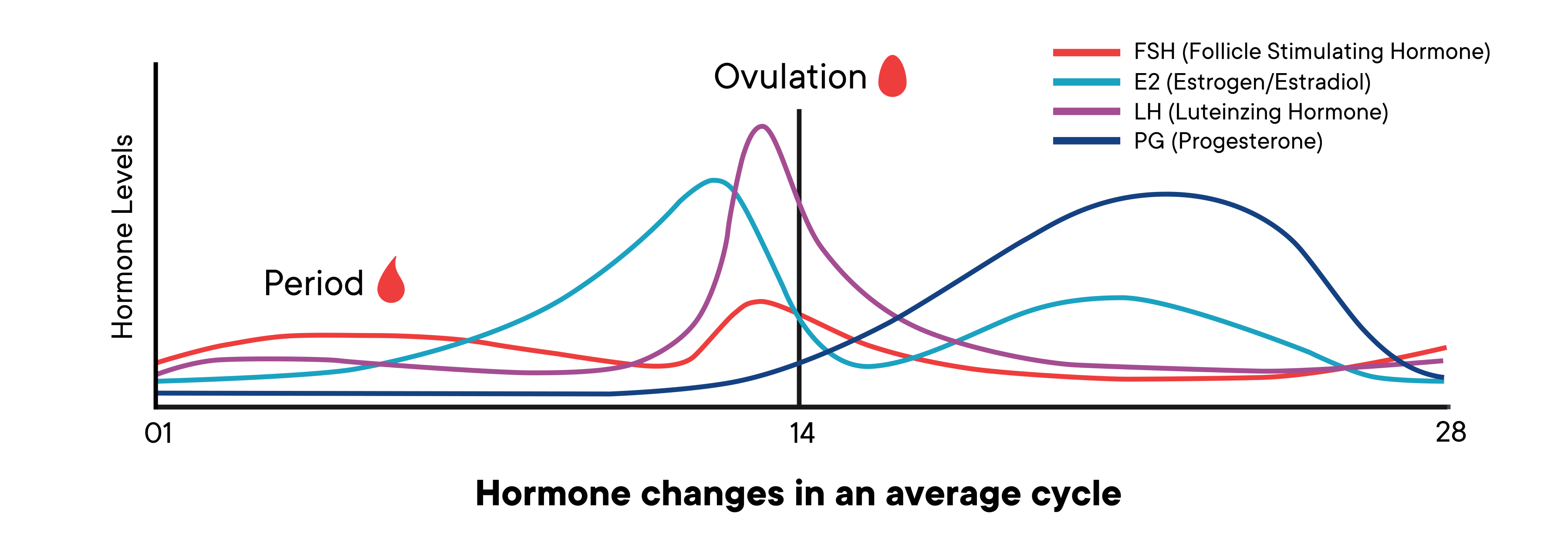
Look at the hormones just after ovulation. Levels of estrogen drop slightly, and then progesterone (and estrogen) start to rise. If there is no hormonal signal that pregnancy has begun, they begin to drop again midway through the luteal phase, eventually triggering the period.
Your ovulation is not a clock
Any factors that influence the hormonal pulsing in your brain can influence your ovulation. Environmental and internal factors like stress, diet, and exercise changes can lead your ovulation to happen slightly earlier, or later, or not at all. Your period may then come earlier or later as well, and be lighter or heavier.
Your follicular phase is considered “plastic," compared to your luteal phase
That means it can commonly change in length, from cycle to cycle. If you know the length of your typical luteal phase (most often 13–15 days) you can count backward to get an idea of when you ovulated. Changes in the length of your cycle are usually pinpointed in the follicular phase—the time it takes a follicle to reach the point of ovulation.
It’s common not to ovulate on a regular basis when you first start menstruating. It’s also common to have irregular ovulation just after pregnancy and breastfeeding, and during the years approaching menopause.
Why does ovulation matter?
Not ovulating every once in a while may not be a concern, but if it becomes common, or if you stop ovulating altogether (and aren’t getting hormones in another way), serious health concerns can arise as a result.
The process of ovulation provides your body with much-needed levels of estrogen and progesterone—hormones that play a role well beyond fertility. They impact your bone density, heart health, metabolism, sleep quality, mental health, and beyond. Getting enough of them is important.
Anovulation during the fertile years is associated with osteoporosis, cardiovascular disease, and certain cancers later in life (22–25). Athletes with menstrual dysfunctions, for example, are significantly more likely to suffer from stress fractures (26).
How do I know if I’m ovulating?
As an adult, you are probably ovulating most of the time if your cycle is generally within range (that’s 24–38 days for adults, with fewer than 7–9 variance cycle-to-cycle, and a menstrual period of 2–7 days) (27). Cycles that are consistently outside of those ranges (they are long, short, or very irregular) can be an indication of anovulation, and a reason to talk to your healthcare provider.
To know if you’re ovulating (and when in your cycle it happens), you might try:
Tracking your cycle length and regularity in Clue
Using ovulation urine tests, bought at your pharmacy
Tracking your physical signs of fertility for a few cycles, including your basal body temperature and cervical fluid
Have your healthcare provider check your hormonal profile (by testing a sample of your blood, taken during your mid-luteal phase)
When do I take an ovulation test?
You can test any time of the day, but it’s best to do it at the same time each day.
Ovulation test kits recommend picking a time when you haven’t urinated for 4 hours before testing or had excessive fluid intake. LH typically rises in the morning, between 4–8 am (29). If you test before it first rises, you may get a negative result that day, but you should still get a positive result the next day. If you’re trying to detect the earliest rise of LH, or if you're having trouble getting a positive result, try testing at different times throughout the day and see what works best for your body.
Article was originally published Nov. 23, 2017